Your basket is currently empty!
A Messy End for TB infected
A Messy End for TB-infected Macrophages
Eicosanoid pathways regulate adaptive immunity to Mycobacterium tuberculosis.
Divangahi, M. et al. (2010). Eicosanoid pathways regulate adaptive immunity to Mycobacterium tuberculosis. Nature Immunology. 11:751-8. [PMID: 20622882]
| More than two billion people (one third of the world’s population) are infected with Mycobacterium tuberculosis, the causative agent for Tuberculosis (TB). It is a leading cause of mortality both in the developing world, and among immunocompromised individuals, such as those with HIV.
Intriguingly, only around 10% of those infected with M. tuberculosis become ill with TB. Professor Sam Behar’s group at Harvard Medical School have been working to establish why. They believe that by understanding the immunological basis for protection from TB onset, they will find new ways to treat M. tuberculosis-infected individuals to prevent disease. Recently, his team published a study showing how M. tuberculosis influences cell death pathways to hide from the immune system. |
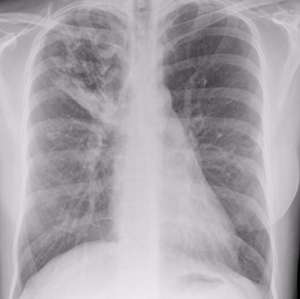 Tuberculosis affects the lungs, causing cavities like the one seen as a white area in the upper left of this x-ray Tuberculosis affects the lungs, causing cavities like the one seen as a white area in the upper left of this x-ray |
In the body, macrophages scavenge for pathogens and engulf them by phagocytosis. M. tuberculosis is able to survive inside macrophages, rather than being destroyed and displayed to the immune system to provoke an immune response. When macrophages die by apoptosis, their contents (including M. tuberculosis if it is present) are distributed neatly into ‘blebs’ or vesicles, which can be taken up by dendritic cells (DC) and again, presented to the immune system. However, M. tuberculosis has a trick up its sleeve: instead of following the apoptotic death pathway, infected macrophages die by necrosis (a more disorganized ending) and the pathogen is able to spread and remain undetected. A factor affecting the choice between necrosis and apoptosis is the availability of eicosanoids. If eicosanoid prostaglandin E2 (PGE2) is available, cells are able to repair membrane disruptions and die by apoptosis, but when PGE2 is lacking, cells must die by necrosis.
The Behar lab worked with mice lacking 5-lipoxygenase, a negative regulator of PGE2 production (Alox5-/- mice) to characterize the immune response to M. tuberculosis. Macrophages from Alox5-/- mice are known to undergo more apoptosis following M. tuberculosis infection, and the mice are consequently more resistant to infection.
Using multimer staining specific for the M. tuberculosis TB10.4 antigen, the team showed that Alox5-/- mice were able to mount a larger, and crucially, faster CD8+ T cell response than wild-type mice.
To study the initiation of CD8+ T cell immunity in more detail, they transferred in vitroinfected Alox5-/- macrophages into wild-type mice. The transferred macrophages were sufficient to completely recapitulate the enhanced immune response, giving a faster and larger CD8+ T cell response.
The team also showed that CD8+ T cell activation induced by M. tuberculosis–infected Alox5-/- macrophages requires antigen presentation by DC. They pulsed macrophages with the ovalbumin peptide epitope SIINFEKL, and then returned them to host mice and measured the subsequent anti-SIINFEKL CD8+ T cell response with Pro5® Pentamer staining. This staining is shown in figure 4 of the paper. As expected, the SIINFEKL response was greater when Alox5-/-macrophages were used. When diphtheria toxin treatment was included in their protocol and used to selectively deplete DC, however, the enhanced response was lost. This finding clearly indicates that T cell activation by M. tuberculosis–infected Alox5-/- macrophages depends on DC.
Presentation of macrophage-derived tuberculosis antigens by DC depends on efficient apoptosis, to ensure that the antigens are passed to DC in apoptotic blebs. When caspase inhibitors were used to block apoptosis in M. tuberculosis–infected Alox5-/-macrophages, the early expansion of TB10.4-specific CD8+ T cells was lost. This shows that an intact apoptosis pathway is central to mounting an efficient T cell response against M. tuberculosis.
By demonstrating exactly how M. tuberculosis can impair host immunity, and linking cell death pathways to the initiation of an effective anti-tuberculosis immune response, the Behar lab have unearthed information that should be helpful in designing the next generation of tuberculosis vaccines.
